
Pancreas Transplant in India: Progress and Future
Introduction
Diabetes is a major public health problem in both developed as well as developing countries. The global prevalence of diabetes is estimated to be around 11% amongst the age group of 20-79 years. Diabetes is one of the leading causes of chronic kidney disease (CKD) and end-stage kidney disease (ESKD) accounting [1] for 50% of cases globally. Pancreas transplant offers the definitive cure for this disease. The first successful pancreas transplant was carried out by WD Kelly in 1966, refinements in surgical techniques and advancements in immunosuppressive therapy over last three decades have greatly improved the results and prognosis of [2] pancreas transplant.
Pancreas transplant is the only treatment that helps to maintain euglycemia and prevents metabolic disturbances which frequently occur in type 1 diabetes patients that persists and even worsen in patients when only kidney transplantation is done. As more and more centres are offering simultaneous pancreas and kidney transplant, 1 year and 5 year survival rates are comparable to other [3] solid organs transplantation.
Indications for pancreas transplant are
- • Severe complications of diabetes mellitus with frequent and severe hypoglycemia or ketoacidosis.
- • Poor quality of life in spite of insulin therapy.
- • Patients with type 1 diabetes with end-stage renal failure on dialysis
Various methods of pancreas transplantation are
- 1. Pancreas transplant alone (PTA)
- 2. Simultaneous pancreas and kidney transplant (SPK)
- 3. Pancreas after kidney transplant (PAK)
- 4. Simultaneous deceased donor pancreas and live donor kidney transplant
SPK is now the first choice of treatment in a patient with type 1 diabetes mellitus and related end-stage renal disease. Pancreas alone transplant can be done in patients with preserved kidney [5] function and hypoglycaemic unawareness.
Islet Cell Transplant
The incidence of islet cell transplantation have reduced after discovery of insulin. There was a realization that apart from the inconvenience of repeated glucose measurements and insulin injections, many patients still had to face the major complications of diabetes. The regimen followed for islet cell transplantation is “Edmonton Protocol” which consists of transplanting an adequate islet mass sometimes from sequential donors (>10,000 islet equivalents per kg recipient body weight), immediate infusion of the islets following isolation, and avoidance of corticosteroids. As in whole pancreas transplantation, the islets can be transplanted [6] alone or after kidney transplantation.
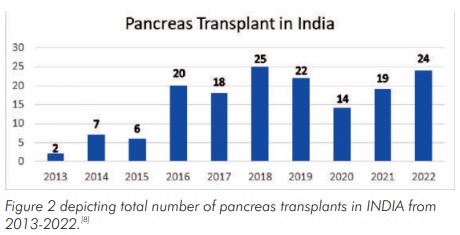
Pancreas Transplant in India
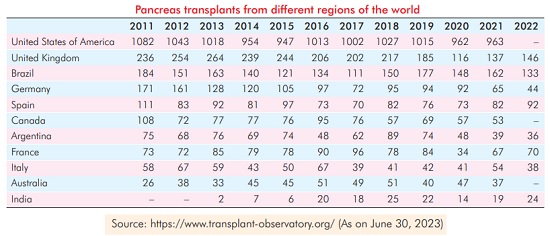
About 1000 pancreas transplants are performed in the USA each year. In contrast to this, less than 100 such transplants have been performed so far in India. At present, only a few centres across the country offer pancreas transplant on a regular basis including Mahatma Gandhi Medical [7] College & Hospital, Jaipur.
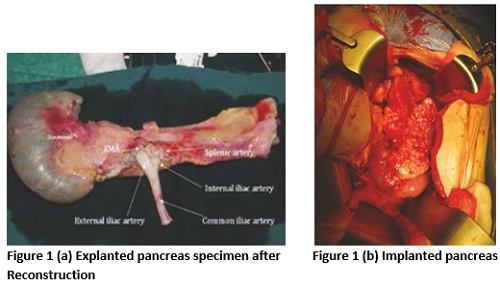
The reasons for lack of pancreas transplantation in our country has been the lack of availability of deceased organ donors. This situation is changing fast with over 900 deceased organ donation in [7] 2022.
Challenges in Indian Settings at Present
Although there is an increase in number of deceased organ donors in India, the number of pancreas transplants are still low. This is because unlike kidney and liver, only a small proportion of all donated pancreas' can be used for transplantation, as criteria for pancreas suitability for transplantation are very stringent like [7] age limit between 10-45 years, obesity etc.
Future in pancreas Transplant
Segmental pancreas transplant from live donors has also been reported. The success of this concept potentially bypasses the issues surrounding organ shortage for waitlisted patients in the same way as in live kidney/liver transplant. With technological advancement, the new devices to improve blood glucose monitoring and insulin therapy are being developed to reduce the risk of wide fluctuations in blood sugars. An artificial pancreas also known as closed-loop insulin delivery systems use a continuous glucose monitoring that measures interstitial glucose concentration, an insulin pump, and a control algorithm to calculate insulin dose and maintain normoglycaemia without user [9] input.
Other Recent Advances in Pancreas Transplant
Advances over the last decade suggest that generating functional beta-cells from stem cells is achievable. However, there are aspects of beta-cell development including the signalling pathways that instruct endocrine progenitor cells to differentiate into mature and functional beta-cells which remain poorly understood. These ideas combined with ideas of biological printing using the extracellular matrix as a scaffold to recreate a new biological pancreas are exciting, and although have their own challenges may change the [10] way transplant is performed.
Conclusion
Pancreas transplant in association with simultaneous kidney transplant is growing and has quickly become the gold standard of care for patients with type 1 diabetes mellitus and renal failure. Significant improvements in quality of life and increase in life expectancy make pancreas transplant an economically viable option. It remains the most effective method of establishing and maintaining euglycemia, halting and potentially reversing complications associated with diabetes mellitus.
References
- 1. Hoogeveen EK. The Epidemiology of Diabetic Kidney Disease. Kidney and Dialysis. 2022;2(3):433-442. https://doi.org/10.3390/kidneydial2030038.
- 2. Scalea JR, Pettinato L, Fiscella B, Bartosic A, Piedmonte A, Paran J, Todi N, Siskind EJ, Bartlett ST. Successful pancreas transplantation alone is associated with excellent self-identified health score and glucose control: A retrospective study from a high-volume center in the UnitedStates. Clin Transplant. 2018 Feb;32(2).
- 3. Meirelles Juń ior RF, Salvalaggio P, Pacheco-Silva A. Pancreas transplantation: review. Einstein (Sao Paulo). 2015 Apr-Jun;13(2):305-9.
- 4. Dholakia S, Oskrochi Y, Easton G, Papalois V. Advances in pancreas transplantation. J R Soc Med. 2016 Apr;109(4):141-6.
- 5. Kopp WH, Verhagen MJ, Blok JJ, Huurman VA, de Fijter JW, de Koning EJ, Putter H, Baranski AG, Schaapherder AF, Braat AE, Ringers J. Thirty Years of Pancreas Transplantation at Leiden University Medical Center: Long-term Follow-up in a Large Eurotransplant Center. Transplantation. 2015 Sep;99(9):e145-51.
- 6. Mehta N Naimish, Sinha Sanjay, Friend Peter, Pancreas Transplantation, Current Pancreatic surgery 2019: 157-178.
- 7. https://www.organindia.org/ORGAN-DONATION/pancreas-transplantationindia/.
- 8. https://notto.mohfw.gov.in/WriteReadData/Portal/News/806_1_data_2022.pdf.
- 9. Abdulrahman O Al-Naseem and others, Pancreas transplantation today: quo vadis?, European Journal of Endocrinology, Volume 188, Issue 4, April 2023, Pages R73-R87, https://doi.org/10.1093/ejendo/lvad032.
- 10. Yagi H, Soto-Gutierrez A, Kitagawa Y. Whole-organ re-engineering: a regenerative medicine approach in digestive surgery for organ replacement. Surg Today 2013; 43: 587-594.
- Mehta NN, Akhani MK, . Pancreas Transplant in India: Progress and Future. Indian Transplant Newsletter. Volume 22 Issue 1, April 2023 - June 2023
- Mehta NN, Akhani MK, . Pancreas Transplant in India: Progress and Future. Indian Transplant Newsletter. Volume 22 Issue 1, April 2023 - June 2023. Available at:
https://www.itnnews.co.in/indian-transplant-newsletter/issue68/Pancreas-Transplant-in-India-Progress-and-Future-1229.htm
